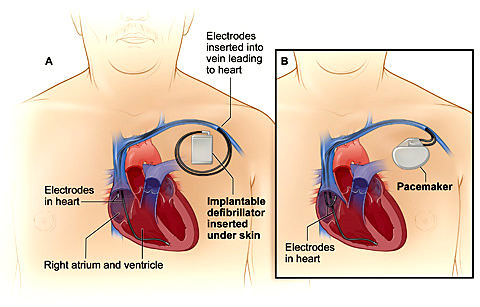
The Implantation of cardiac pacing devices in children and young adults can be challenging and different from the adult population due to their smaller size, their longer life expectancy, and anatomical variations associated with congenital heart defects.
Knowledge of indications, pacing leads and devices, anatomical variations, and the technical skills are important for those who implant and care for children with pacemakers.
Pacing in children is mainly performed in the setting of congenital or post-surgical complete heart block and less frequently in some surgical patients with sinus node dysfunction.
The indications, anatomical variations, and technical skills required for pacing children are different compared to those for adults. Also, current pacemakers are smaller sized, have longer battery life, multiple programming options, and therapeutic capabilities, and therefore provide greater options for pacing in children.